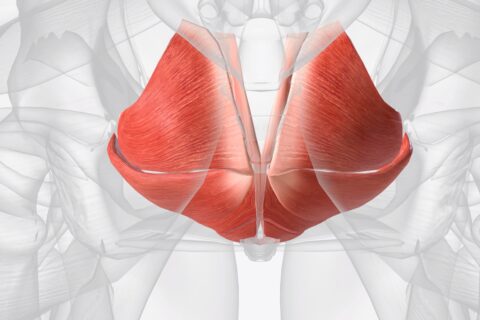
Chronic heel pain can plague many athletes. With the help of a few therapeutic movements and treatments, you can try to relieve your plantar fasciitis symptoms.
Chronic heel pain can plague many athletes. With the help of a few therapeutic movements and treatments, you can try to relieve your plantar fasciitis symptoms.